Search
Operating Department Practice BSc (Hons)
Study level: Undergraduate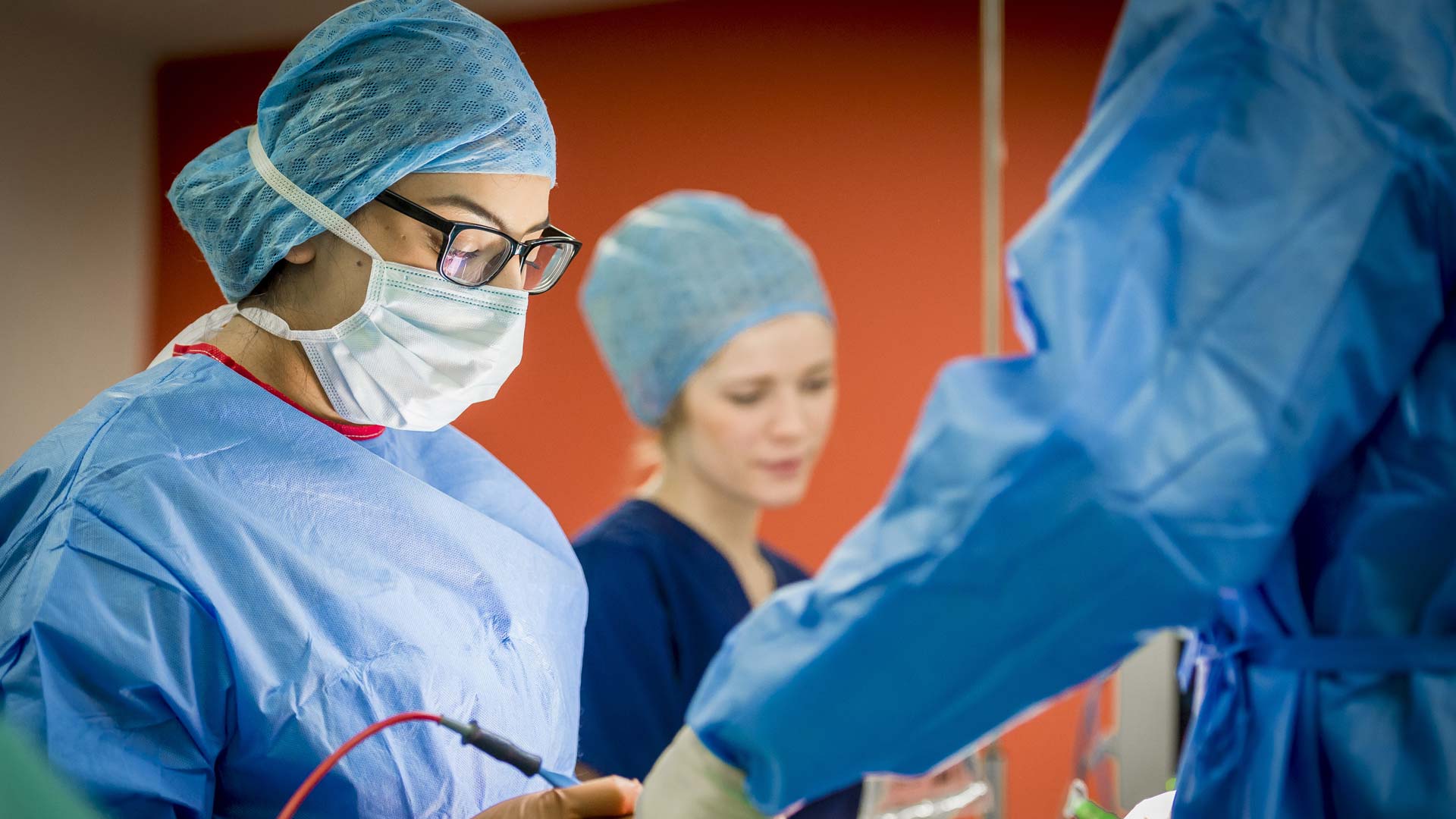
Operating Department Practice (ODP) is an exciting and rewarding career where you work within the perioperative theatre environment caring for patients undergoing surgery.
Course features
Course option
Year of entry
Location
Coventry University (Coventry)
Study mode
Full-time
Duration
3 years full-time
UCAS codes
HU10
Start date
September 2026
Course overview
Operating Department Practitioners (ODPs), unique among undergraduate Allied Health Professions in the UK, receive specialised training for operating theatre roles. Throughout your training, you'll develop autonomy as a practitioner, collaborating with anaesthetists, surgeons, and other professionals to prepare and assist in surgical and anaesthetic procedures, thereby enhancing patient care experiences.
Operating Department Practitioners (ODPs) play a crucial and unique role in patient care. They are responsible for a wide spectrum of tasks essential for the smooth running of perioperative environments. As an ODP you may prepare and maintain operating theatres, ensure the availability of equipment and drugs, manage patient safety and support patients' emotional and physical needs throughout their surgical journey, from pre-anaesthesia to post-anaesthetic care in recovery. Staying calm in pressured environments, ensuring safety and ensuring everyone has a voice to speak up when needed are all vital skills you’ll be developing on the course.
- Leads to eligibility to apply for registration with the Health and Care Professions Council (HCPC) for registration as an ODP (please see Accreditation section for more information).
- You will learn through simulated activities such as role play and clinical skills development. Facilities replicate those found in hospitals, including a mock operating theatre and scrub room, mock ward setting, high dependency bays, and utilising high-tech manikins which respond to the treatment provided4.
- Learn to collaborate and thrive as an ODP and within multidisciplinary teams to coordinate safe, evidenced-based care delivery.
- Practice placements sourced for you by the university, providing you with opportunities to develop clinical skills and become a safe, confident and competent practitioner2,5.
- Study one academic module at a time, with five weeks of learning followed by one week of assessment per module.
- All eligible students on this course can apply for a minimum payment from the government of £5,000 per year. You can apply for additional payments if you incur childcare costs6.
Rated Gold Overall
Teaching Excellence Framework (TEF) 20235 QS Stars for Teaching and Facilities
QS Stars University RatingsTop 5 Student City in England (Coventry)
QS Best Student Cities Index 2026Why you should study this course
Careers in operating department practice enable you to develop a mix of technical, management and communication skills to support a diverse range of patients during their most vulnerable moments.
- The role of ODPs is dynamic and varied. Increasingly, ODPs are also adapting their knowledge and skills to work in non-traditional acute settings like emergency departments, intensive care, interventional radiology, cardiac catheterisation, MRI, CT scanning, and endoscopy units.
- Teaching and learning are supported by highly trained, clinically current and experienced staff, clinical partners, service users, fellow ODP students and those from other health courses across the school.
- We focus on your future employability, offering you insight into roles in areas such as surgical first assistance, critical care, leadership and management.
Studying in the School of Health and Care
Gain the skills and experience to transform lives, communities and the future of healthcare delivery. We aim to empower you to become a stand-out healthcare professional, capable, competent and confident in your field and role within the wider healthcare team.
While continuously developing your sense of professional identity as an operating department practitioner from day one, you'll also collaborate with learners from other School of Health and Care fields, learning in an environment that puts inclusivity, diversity and dignity at its heart.
Accreditation and professional recognition
The degree is accredited1 and recognised by the following bodies:

Health and Care Professions Council (HCPC)
The Operating Department Practice BSc (Hons) programme is approved by the Health and Care Professions Council (HCPC).
On successful completion of the programme, you will be eligible to apply for HCPC registration (subject to HCPC criteria and any additional costs. See the website for full details).1

College of Operating Department Practitioners
The degree is currently accredited by the College of Operating Department Practitioners1. Following changes that have been made to improve the course, we will apply for re-accreditation for entrants of 2025-26. If any changes occur with respect to our accreditation, we will notify applicants and students as soon as possible. This is a normal part of the process of continuous improvement of our courses to ensure they remain up-to-date and reflect best practice.
What you'll study
During your degree, you will study:
- professional practice
- surgical practice
- anaesthetic practice
- post-anaesthetic practice
- critical care and non-elective practice
- clinical leadership and management
- practice development
- complex practice
- reflective and research-based practice.
We regularly review our course content, to make it relevant and current for the benefit of our students. For these reasons, course modules may be updated.
How you'll learn
We understand that everyone learns differently, so this course will consist of structured teaching sessions which can include:
- on-campus lectures, seminars and workshops
- group work
- self-directed learning
- clinical placement opportunities2,5.
Teaching contact hours
As a full-time undergraduate student, you will study modules totalling 120 credits each academic year. A typical 20 credit module requires a total of 200 hours study. This is made up of teaching contact hours, guided and independent study.
Teaching hours
Teaching hours vary each semester, year of study and due to module selection. During your first year you can expect 15-18 teaching hours each week. You will also have the option to attend optional sessions including time with a progress coach or to meet with staff for advice and feedback. As you progress through your studies, teaching hours may reduce.
Practice-based learning
Practice-based learning forms an essential and significant part of your learning experience. Practice hours will differ between placements and different health and care courses. You will have access to university staff, but should expect to spend the majority of your contact time with practice collaborators undertaking placement activity. Overall, the hours you undertake in practice-based learning will need to satisfy the eligibility requirements set by the professional body regulating the profession, the HCPC. No less than 2112 practice-based hours gained from a combination of placement and simulated learning will need to be completed over the course of your degree.
Guided and independent study
Throughout your studies, you will be expected to spend time in guided and independent study to make up the required study hours per module. You'll be digging deeper into topics, review what you've learnt and complete assignments. This can be completed around your personal commitments. As you progress through your studies, you'll spend more time in independent study.
Online learning
As an innovative university, we use different teaching methods including online tools and emerging technologies. So, some of your teaching hours and assessments may be delivered online.
Assessment
This course will be assessed using a variety of methods which will vary depending upon the module. Assessment methods may include:
- coursework
- practice placement2,5
- formal examinations
- Virtual Simulated Placements
- simulations
- Objective Structured Clinical Examinations
- presentations.
The Coventry University Group assessment strategy ensures that our courses are fairly assessed and allows us to monitor student progression towards achieving the intended learning outcomes.
Entry requirements
Typical entry requirements:
Not got the required grades? We offer this degree with an integrated foundation year.
Fees and funding
| Student | Full-time | Part-time |
|---|---|---|
| UK, Ireland*, Channel Islands or Isle of Man | £9,790 per year | Not available |
| EU | £9,790 per year with EU Support Bursary** £20,800 per year without EU Support Bursary** |
Not available |
| International | £20,800 per year | Not available |
A non-repayable grant of £5,000 and extra payments worth up to £3,000 may be available to eligible students for each year of study6. Read more about this in the NHS Learning Support Fund information booklet.
For advice and guidance on tuition fees and student loans visit our Undergraduate Finance page and see The University’s Tuition Fee and Refund Terms and Conditions.
The University will charge the tuition fees that are stated in the above table for the first Academic Year of study. The University will review tuition fees each year. For UK (home) students, if Parliament permits an increase in tuition fees, the university may increase fees for each subsequent year of study in line with any such changes. Note that any increase is expected to be in line with inflation.
For international students, we may increase fees each year, but such increases will be no more than 5% above inflation. If you defer your course start date or have to extend your studies beyond the normal duration of the course (e.g. to repeat a year or resit examinations) the University reserves the right to charge you fees at a higher rate and/or in accordance with any legislative changes during the additional period of study.
We offer a range of International scholarships to students all over the world. For more information, visit our International Scholarships page.
Tuition fees cover the cost of your teaching, assessments, facilities and support services. There may be additional costs not covered by this fee such as accommodation and living costs, recommended reading books, stationery, printing and re-assessments should you need them. Find out what's included in your tuition costs.
The following are additional costs not included in the tuition fees:
- Any optional overseas field trips or visits: £400+ per trip.
- Any costs associated with securing, attending or completing a placement (whether in the UK or abroad).
*Irish student fees
The rights of Irish residents to study in the UK are preserved under the Common Travel Area arrangement. If you are an Irish student and meet the residency criteria, you can study in England, pay the same level of tuition fees as English students and utilise the Tuition Fee Loan.
**EU Support Bursary
Following the UK's exit from the European Union, we are offering financial support to all eligible EU students who wish to study an undergraduate or a postgraduate degree with us full-time. This bursary will be used to offset the cost of your tuition fees to bring them in line with that of UK students. Students studying a degree with a foundation year with us are not eligible for the bursary.
Facilities
Develop your skills and knowledge using our cutting-edge simulation facilities. These include mock operating theatre, simulated ward settings, high dependency bays and the use of advanced manikins4.
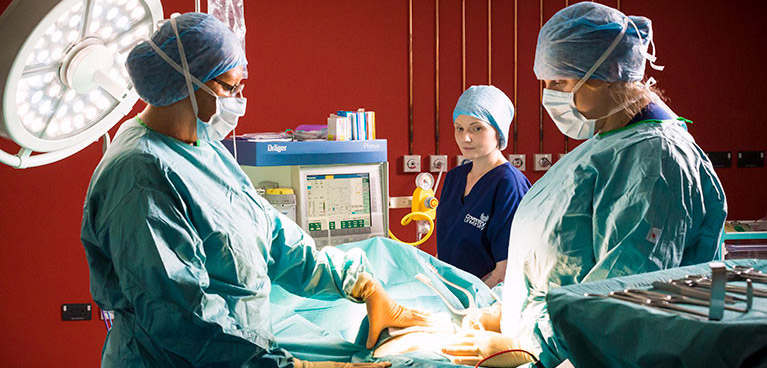
Mock operating theatre
Our operating theatre is set up to accommodate procedures that would take place during hospital surgery. It includes a scrub room and the machines, equipment and lighting you will need to use to be an effective operating department practitioner.

Alison Gingell Building
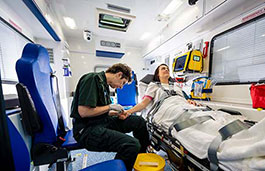
Our state-of-the-art Alison Gingell Building features a mock ambulance, high-tech manikins, hospital wards, critical care settings and therapy suites. This gives you the opportunity to learn in situations that mirror real life scenarios.

Mock hospital wards
We have two fully-equipped mock hospital wards, each containing 4 beds. The wards are built to NHS standards and contain moveable beds, first aid equipment and patient monitoring tools, so that you can study a complete patient pathway.
Facilities are subject to availability4. Access to some facilities (including some teaching and learning spaces) may vary from those advertised and/or may have reduced availability or restrictions where the university is following public authority guidance, decisions or orders.
Careers and opportunities
Multiple pathways for professional development and progression are available for ODPs. Beyond the core role, career progression may lead to specialised roles such as Surgical First Assistant, Surgical Care Practitioner, Anaesthetic Associate, or Emergency Care Practitioner. Other opportunities exist in management, practice, and education within the field of ODP, allowing you to continually expand your skills and contribute to the advancement of perioperative care.
Where our graduates work
Previous graduates of this course have gone on to work for the the NHS, private healthcare companies, global medical technology companies, universities and the Royal Navy, Army and the RAF.
How to apply
You may also like

Adult Nursing BSc (Hons)
Children and Young People's Nursing BSc (Hons)